
Future depression treatment may not take the form of a bottle of pills. Non-invasive neuromodulation interventions from startups like Neurolief and Flow Neuroscience are already approved for patients who do not respond adequately to antidepressants. Yet more experimental approaches are also gaining ground, including implantable systems designed to deliver stimulation in a more continuous and embedded way.
Inner Cosmos is part of that emerging layer. The company is developing a miniaturized implanted system for people with treatment-resistant depression, a group that often faces major practical barriers once first-line treatments fail. Even when advanced options such as TMS are available, access can require daily clinic visits over multiple weeks. For patients already dealing with severe depressive symptoms, that burden can become part of the problem. Inner Cosmos is building around that gap with a minimally-invasive implant.
Inner Cosmos is developing a minimally invasive brain-computer interface designed to treat depression through targeted neurostimulation. The system centers on a small implant placed beneath the scalp, where it delivers electrical stimulation to brain regions involved in mood regulation. Unlike more invasive neurotechnology systems, it is designed to avoid entering the skull or brain tissue, while still offering a more direct interface than external wearables.

The device targets the left dorsolateral prefrontal cortex, a region commonly associated with mood regulation and executive function and already well established in depression-related neuromodulation. Rather than being implanted in the brain itself, the stimulator is positioned beneath the skin of the scalp in a short outpatient procedure and remains outside the skull, resting on the bone. This extracranial design is central to the company’s risk profile. It offers a more direct and stable interface than a headset placed over hair and skin, while avoiding the surgical burden associated with intracranial implants.
The system is built around a two-part architecture consisting of a small passive implant placed beneath the scalp, and an external power pod that attaches magnetically over it. The implant remains under the hair, while the external pod supplies power and controls stimulation during treatment sessions.
When a session begins, typically once per day, the patient places the pod onto the scalp. The pod wirelessly powers the implant, which then delivers programmed electrical stimulation. Keeping the battery and processing components outside the body allows the implanted disc itself to remain thin and relatively simple in design.
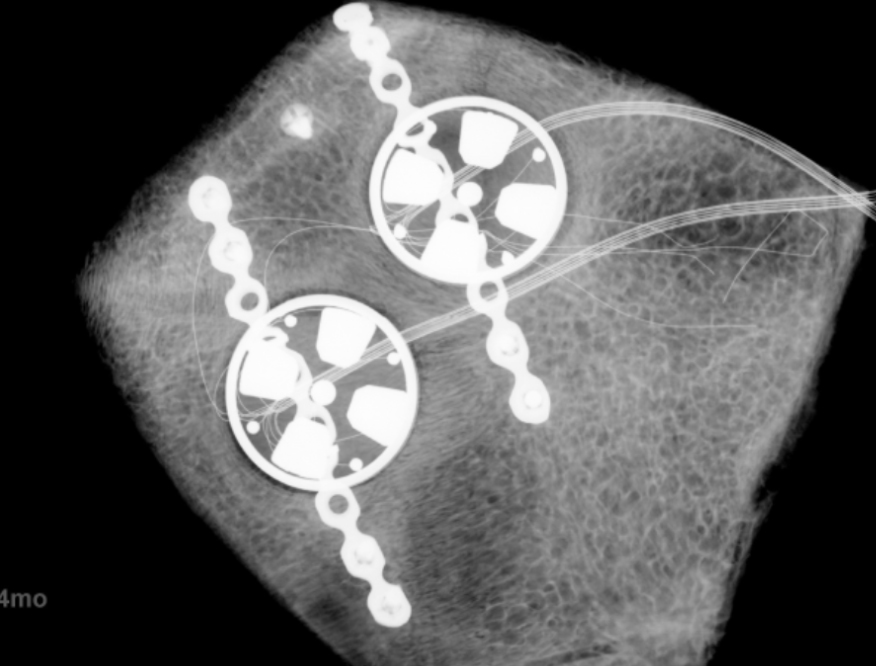
In early 2026, Inner Cosmos completed its early feasibility trial, publishing results from its multi-year psychiatric neurostimulation study. The early data already appears promising in terms of efficacy, with patients reporting meaningful and sustained improvements in mood. In one clinical update, a participant saw their depressive symptoms reduced by 54%.
More notably, that result was reported to be 21% better than the best response the same individual had previously achieved with hospital-based treatments such as TMS. The finding points to an important idea underlying Inner Cosmos’s approach–smaller, consistent daily stimulation delivered at home may in some cases outperform more intensive but less frequent clinic-based interventions. The broader logic is tied to neuroplasticity, with repeated stimulation intended to support gradual changes in brain function over time.
Still, the longer-term questions matter as much as the early clinical signals. One of the clearest next steps for Inner Cosmos is the move toward a closed-loop system. At present, stimulation levels are set by a clinician based on patient response. Over time, that model could become more adaptive, with the device using neural data to detect changes in state and adjust stimulation accordingly.
That closed-loop possibility also raises more difficult questions. If a device is continuously shaping mood, where does treatment end and modulation begin? Some patients may experience that as a return to themselves rather than a disruption of identity, particularly if the technology helps reduce the burden of depression. Even so, questions around agency, autonomy, and the boundaries of algorithmic intervention are likely to become more important as these systems grow more sophisticated.
Beyond the ethical dimension, there is also the commercial one. For a system like this to scale, Inner Cosmos will need more than technical validation or regulatory progress. It will also have to make a convincing case to payers that an implanted, device-based treatment can be justified economically relative to existing standards of care. The neuromodulation for depression space is heating up. And so, as the company moves toward pivotal clinical trials, that cost-effectiveness argument may become just as important as the clinical data itself.
Inner Cosmos does not represent the arrival of a new psychiatric mainstream yet, but it does point to where part of the field may be heading. Its model brings together several ideas that increasingly define next-generation neurotechnology: miniaturization, home-based care, and a tighter link between intervention and everyday life.
[Image credit: Inner Cosmos]